Hypnosis as part of a new framework for treating pain (06/01/2011)
 Professor Mark Jensen has published a review of psychological treatments for pain which organises different modalities into a framework. Currently, models which explain why one treatment works for pain do not necessarily help us to understand the mechanisms behind other pain treatments. The reason for creating an overall framework is to better understand how different treatments work, to understand why treatments work differently for different patients, and to understand how different treatments fit together.
Professor Mark Jensen has published a review of psychological treatments for pain which organises different modalities into a framework. Currently, models which explain why one treatment works for pain do not necessarily help us to understand the mechanisms behind other pain treatments. The reason for creating an overall framework is to better understand how different treatments work, to understand why treatments work differently for different patients, and to understand how different treatments fit together.
In the paper he considers eight major psychosocial treatments for pain:
- hypnosis
- relaxation
- mindfulness meditation training (MMT)
- operant treatment
- graded exposure in vivo
- motivational interviewing
- cognitive and cognitive-behavioral therapy (CBT)
- acceptance-based CBT (ACT)
These treatments are then organised according to:
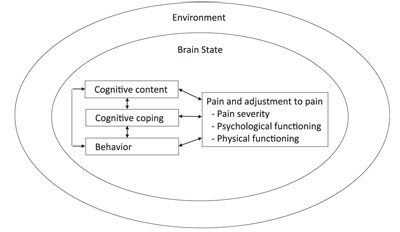
- Environmental factors - responses of people around the patient (e.g. do they reinforce pain behaviours, or do they try to motivate change?)
- Brain states - changes in executive function or dissociation are thought to be associated with the experience of pain, and can be altered with hypnosis and probably via other mechanisms too
- Cognitive content - what patients believe about their pain
- Cognitive coping - cognitive strategies patients use for managing pain and mood
- Behaviour - what patients do about their pain, or in response to their pain?
Different treatments tend to target different components of the model. For instance, when a patient believes that movement will make their pain worse (maladaptive cognitive content) and decides to rest until the pain goes (maladaptive behaviour), then the therapist might decide to use psychoeducation about pain to alter the cognitive content, and encourage graded increases in movement (behavioural treatment). Alternatively, a therapist using hypnosis might create changes in the patient's brain state, and give suggestions for pain relief which affect how the patient feels about their pain (which would affect the cognitive coping dimension).
One interesting aspect of the model is the comparison that is made between hypnosis and mindfulness meditation. These are often seen as quite separate treatments, with hypnotic treatments and suggestions aiming to modify cognitive content, whereas mindfulness is about non-judgementally accepting cognitions and experiences. However, Jensen argues that mindfulness can be seen as similar to the induction phase of hypnosis followed by suggestions for increases in acceptance. Similarly, relaxation can be viewed as an initial phase of hypnosis, leading to similar brain states, but absent the suggestion component.
The upshot of the model is that it gives researchers a useful way to categorise psychosocial treatments for pain, and encourages clinicians to make sure they have more 'arrows to their bow' in order to be able to offer patients a full range of treatments to meet their needs.
Jensen MP. Psychosocial approaches to pain management: An organizational framework. PAIN (2010), doi:10.1016/ j.pain.2010.09.002
Read the abstract at PAIN (the full article is behind a paywall, so to read it all you'll need access to the journal or will have to contact the author)
What is hypnosis?
Definitions of hypnosis
Types of suggestion
FAQ
Scientific theories of hypnosis
History of hypnosis
Animal hypnosis
Key people in hypnosis
Demand characteristics
Scientific research
States of consciousness
Neuroscience
Modification of suggestibility
Attention and hypnosis
Pain research
Hypnosis as a research tool
Genes and hypnotizability
What is hypnotherapy?
Is it effective?
Finding a therapist
Depression
Irritable bowel syndrome
Pain
PTSD
Smoking
Surgery
Weight loss
Hypnosis research papers
Suggestibility scales
Scripts
Videos
Forum
Organisations
Journals
Book reviews
© 2007-2019 Dr Matthew Whalley
